If you have been told you might need a knee or hip replacement, you are probably also being told two other things at the same time: that the surgery has gotten dramatically better in the last twenty years, and that it is still major surgery. Both are true. Modern joint replacement is one of the most reliably successful operations in all of medicine, and it is also a procedure that takes months to fully recover from and permanently alters the joint.
The question for many patients is not whether joint replacement works — it does — but whether they have already exhausted the reasonable options short of surgery. Regenerative medicine has changed what “reasonable options” actually means. Below is an honest comparison of the two paths and a framework for thinking about which makes sense for you.
What joint replacement does well
A knee or hip replacement removes the worn joint surfaces and replaces them with metal and polyethylene components. Done well, on the right patient, the results are excellent: dramatic pain relief, durable function, and a return to most daily activities. For patients with end-stage osteoarthritis — bone-on-bone disease, severe deformity, night pain that is no longer controllable — joint replacement is often the right answer, and waiting too long can actually make recovery harder.
That said, joint replacement also has trade-offs. The recovery is real: most patients are looking at twelve weeks of meaningful rehab, with full recovery measured closer to a year. Implants do not last forever — most modern implants are designed for fifteen to twenty-five years of life depending on activity level and patient factors, which is one reason surgeons prefer not to operate too early. There is risk of infection, blood clots, anesthesia complications, and persistent pain in a small percentage of patients. And the joint, once replaced, cannot go back.
What regenerative medicine does well
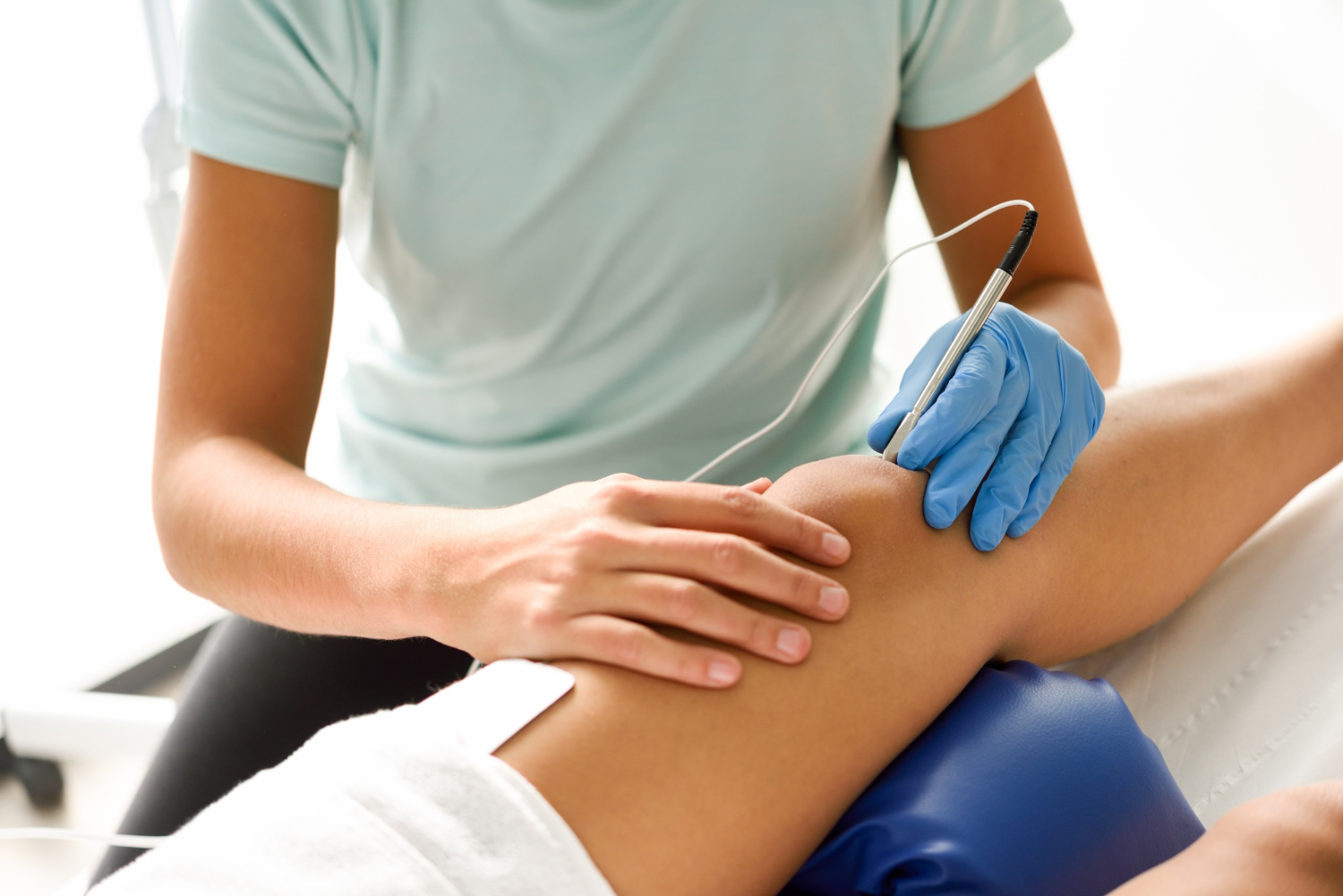
Regenerative medicine takes a different approach. Rather than removing and replacing the joint, the goal is to support the tissue that remains, calm the inflammatory environment that drives pain, and address the mechanical load contributing to the wear. The most established tools in this category include platelet-rich plasma (PRP), bone marrow concentrate, hyaluronic acid, and shockwave or other in-office regenerative devices.
The trade-offs run in the opposite direction from surgery. Regenerative treatments are generally low-risk, performed in the office, and do not require time off your feet. Most patients are back to normal activity within days. The downside is that they are not a permanent solution and they do not work for every patient. They are most effective in mild-to-moderate disease, and they tend to work best as part of a broader plan that addresses the mechanics around the joint, not just the joint itself.
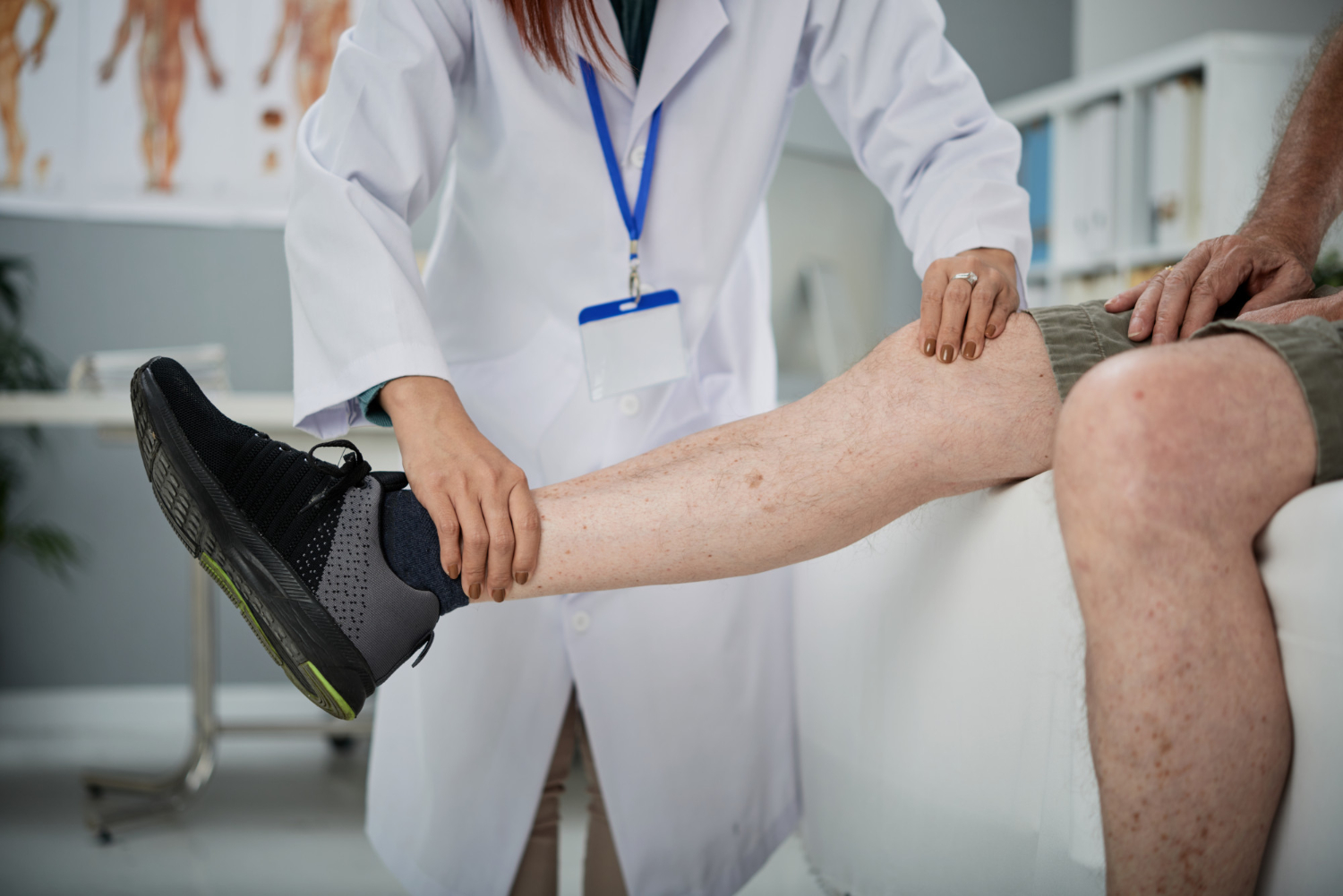
Who is a candidate for which?
There is no clean line, but there are useful guideposts. Patients who tend to do best with regenerative options first include those with:
- Mild or moderate osteoarthritis on imaging — joint space preserved, not bone-on-bone.
- Pain and stiffness that have not yet taken over daily life or sleep.
- A goal of staying active in golf, tennis, pickleball, or training.
- Concerns about anesthesia, blood thinners, or other surgical risk factors.
- A timeline that allows weeks-to-months for treatment to work, rather than needing immediate relief.
Patients who tend to be ready for joint replacement include those with:
- End-stage osteoarthritis with bone-on-bone changes on imaging.
- Pain that has begun to wake them at night or significantly limit walking distance.
- Significant joint deformity or mechanical instability.
- A history of prior treatments — including PRP, cortisone, hyaluronic acid, and PT — that have stopped providing meaningful relief.
- A clear desire to fix the problem definitively rather than manage it.
The most common mistake patients make in this decision
It is not picking the wrong treatment. It is picking too late. Patients who explore regenerative options when they have early or moderate osteoarthritis have a real chance of changing the trajectory of the joint. Patients who wait until they are already bone-on-bone often discover that regenerative treatments cannot do what they hoped, and they end up doing the surgery anyway — having lost a year of function in the meantime.
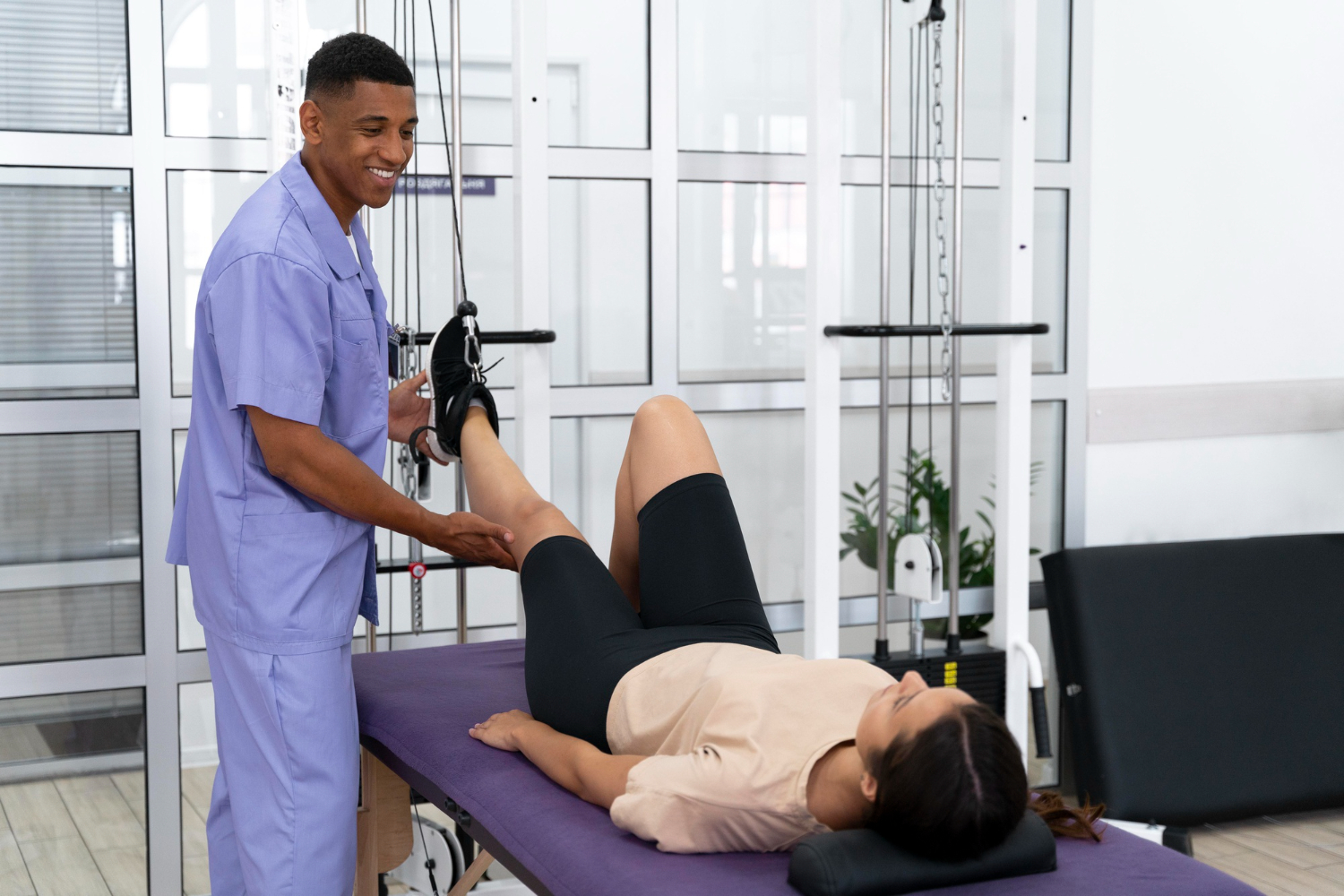
The other common mistake is assuming the choice is binary. It is not. For many patients, the right path is a planned sequence: optimize the mechanics around the joint with proper footwear and orthotics, calm the joint with regenerative treatment, build the surrounding muscles, and then reassess. Joint replacement may eventually be the right answer for some of those patients. For others, a well-managed knee can deliver many more years of activity than they expected.
How a regenerative consultation actually helps
A good consultation is not a sales pitch for whichever treatment the office happens to perform. It is an honest, image-supported conversation about where your joint actually is on the disease spectrum, what your goals are, and what realistic options exist. We routinely tell patients that they are a strong candidate for regenerative treatment — and we routinely tell other patients that surgery is genuinely the right next step and we are happy to refer them to the appropriate orthopedic surgeon.
That kind of clarity is what most patients are actually looking for. The cost of an honest conversation is much smaller than the cost of choosing the wrong treatment for the wrong stage of disease.
Schedule a regenerative consultation in Palm Beach
If you are weighing surgery and want a thoughtful second opinion before you commit — or you have been told to “come back when it gets worse” and you would rather not wait — we offer regenerative consultations at our Palm Beach office. Bring any recent imaging you have. Call to schedule, or request a consultation online.