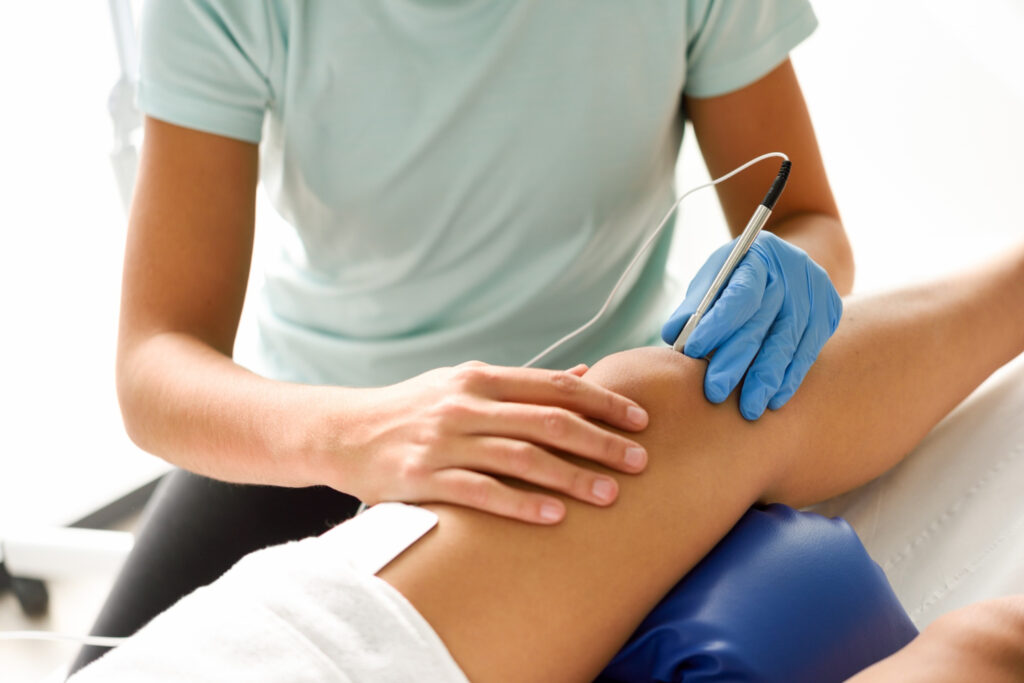
Knee pain has a way of slowly narrowing your life. The walks get shorter, the tennis match becomes the round of golf, the round of golf becomes a cart ride, and eventually even the stairs at home start looking different. By the time most patients sit down with us, they have already cycled through anti-inflammatories, a couple of cortisone injections, maybe a course of physical therapy, and a recommendation to consider knee replacement that they are not ready for.
Platelet-rich plasma — better known as PRP — sits in the space between conservative care and surgery. It is one of the most studied and most widely used regenerative treatments for knee osteoarthritis, and for the right patient it can meaningfully change how the joint feels and functions without committing to a major operation.
What PRP actually is
Platelets are best known for clotting blood, but they also carry a dense concentration of growth factors and signaling proteins. Those proteins are what the body uses every day to direct healing — to call in repair cells, modulate inflammation, and signal local tissue to maintain itself.
PRP is made from a small sample of your own blood, drawn the same way as a routine lab draw. The sample is processed in a centrifuge to separate and concentrate the platelets. The resulting concentrate — many times more potent than the platelets circulating in your bloodstream — is then injected, under image guidance, directly into the affected joint.
Because PRP is autologous (made from your own blood), the risk of rejection or allergic reaction is essentially zero. There is no synthetic medication, no donor tissue, and no foreign substance involved.
Why patients with knee osteoarthritis consider it
Standard treatments for knee osteoarthritis tend to address symptoms rather than the joint environment itself. Anti-inflammatory medications quiet pain but can be hard on the stomach, kidneys, and cardiovascular system over time. Cortisone injections often provide rapid relief, but repeated cortisone in the same joint has been associated with cartilage thinning when overused. Hyaluronic acid injections can be helpful but tend to wear off over months.
PRP works differently. Rather than masking pain or temporarily lubricating the joint, it delivers a concentrated dose of the body’s own signaling proteins into the joint, with the goal of calming inflammation in the synovial environment and supporting the tissue that remains. For many patients with mild-to-moderate osteoarthritis, the result is meaningful, durable improvement in pain and function.
PRP is not a cure for osteoarthritis, and it does not regrow a cartilage surface that has been worn down to bone. Patients who understand that going in tend to be the most satisfied with the results.
Who is a good candidate?
PRP tends to work best for patients who:
- Have mild-to-moderate knee osteoarthritis on imaging.
- Still have functional cartilage to work with — not bone-on-bone end-stage disease.
- Have ongoing inflammation, swelling, and activity-limiting pain.
- Want to delay or avoid joint replacement surgery.
- Have not gotten the results they wanted from physical therapy or cortisone alone.
It can also be useful in early-stage osteoarthritis, post-injury knees, and as part of a broader recovery strategy in active adults who want to keep training. Patients with active infection, certain blood disorders, or active cancer in the area are generally not candidates. A proper consultation determines the right fit.
What a PRP visit looks like
The visit itself is straightforward. After a focused exam and a review of any imaging, a small amount of blood is drawn — typically the volume of two or three vials of routine lab work. The blood is processed in our office using a sterile, closed system. While the centrifuge runs, the knee is prepped and numbed.
The injection itself is performed under ultrasound guidance to make sure the PRP reaches the right space inside the joint. Most patients describe brief pressure rather than significant pain. The whole appointment usually takes about an hour.
Some soreness, swelling, and stiffness in the knee for the first few days after PRP is normal and expected — that is the inflammatory phase the treatment is designed to trigger. Anti-inflammatory medications are usually held for a short period before and after the injection so they do not blunt the effect.
What to expect over the weeks that follow
PRP does not work like cortisone. Cortisone shuts pain down quickly and the relief is often felt within a day. PRP works gradually, over weeks, as the local tissue environment responds. Most patients begin to notice changes by the four- to six-week mark, with continued improvement for several months after that.
Some patients respond strongly to a single injection. Others benefit from a short series spaced several weeks apart. The plan is individualized, not one-size-fits-all.
PRP works best when it is paired with the rest of the picture: a targeted strengthening program, weight optimization when relevant, footwear and orthotic review, and addressing any biomechanical contributors that drove the cartilage wear in the first place. A joint injection alone, without addressing the load going through that joint, tends to produce shorter-lived results.
Schedule a PRP consultation in Palm Beach
If you are in that frustrating space between cortisone and surgery — or you simply want to understand whether regenerative options could change the conversation — an in-office consultation is the right next step. We will review your imaging, examine the knee carefully, and lay out a realistic plan based on the stage of arthritis you actually have, not a generic recommendation. Call our Palm Beach office, or request a consultation online.